Breaking Bottlenecks in Utilization Management
Utilization Management (UM) remains a fundamental component of health plan operations—ensuring that care is medically necessary and delivered efficiently. However, legacy systems and manual processes continue to impede decision speed, inflate administrative costs, and undermine provider and member satisfaction. Health plan executives are under mounting pressure to modernize these workflows. This article examines two key chokepoints in UM and outlines how automation and artificial intelligence (AI) can reengineer the process for better outcomes.
Fragmented Intake Channels: An Unresolved Legacy
Despite significant investments in digital infrastructure, most prior authorization (PA) requests still arrive through outdated, unstructured channels—faxes, phone calls, emails, scanned PDFs, or even smartphone photographs. These formats demand manual transcription and interpretation, driving up labor costs and introducing errors.
According to the CAQH, only 31 percent of prior authorization transactions were processed fully electronically via ASC X12N278, while 37 percent remained fully manual—processed by phone, fax, mail, or email1. Manual processing is considerably more expensive and time-consuming. The CAQH Index shows payer-side costs average $3.50 per manual PA, compared to just $0.05 for fully electronic transactions. On the provider side, each manual submission consumes approximately $10–11 in staff effort2.
This fragmentation affects the downstream UM workflow. Staff must sort through entries, clarify ambiguities, and reconcile incomplete information—all of which extend turnaround times. Providers frequently complain of submitting faxes or emails only to receive phone calls requesting additional details days later. For health plans, this creates backlogs, missed performance targets, and strained provider relations.
Documentation Overload: Reviewing the Irrelevant Along with the Relevant
Once intake is complete, UM nurses face another critical challenge: the volume of clinical documentation submitted in support of authorization requests. Providers often send extensive electronic medical record printouts, diagnostic reports, test results, and specialist notes—sometimes totalling hundreds of pages per case.
Reviewers must manually scan these documents, identify relevant facts, cross-check coverage guidelines, and reach a clinical determination. The process varies significantly in duration, often ranging from 30 minutes to several hours per case. In workloads of 20+ cases per day, this becomes a considerable staff burden.
From the health plan perspective, these delays translate into higher appeal volumes and compliance risks. When documentation is inconsistent or unnecessarily voluminous, decision-making becomes harder to standardize, resulting in variance across reviewers and potential errors that attract regulatory attention.
Automation at Intake: Converting Chaos into Standardized Data
The advent of Intelligent Document Processing (IDP) and Natural Language Processing (NLP) transforms how unstructured intake is handled. These tools can extract structured data from faxes, PDFs, and images, identifying key fields—member demographics, diagnosis codes, CPT codes, dates of service—and automatically populating intake systems.
Phone-based submissions can be converted to text via speech-to-text and NLP solutions. The value is not in eliminating humans, but in creating a single, reliable digital intake stream.
Health plans that implement these tools report dramatic improvements. One regional insurer processed over 200,000 authorizations annually through automated systems, achieving 90 percent first-pass accuracy and reducing data-entry burden by 40 percent. These gains support compliance with evolving CMS mandates on electronic prior authorization standards3.
AI-Infused Clinical Review: Enabling Smarter Decision-Making
Automation’s benefits extend into the clinical review phase when AI-driven tools analyze and summarize documentation. Models trained on medical language and entitlement policies can identify prescribed treatments, prior interventions, labs, and imaging outcomes relevant to PA criteria.
This allows for a triaged review model: routine, low-complexity requests may be auto-approved; ambiguous or high-risk requests are flagged for clinical review. Clinicians are presented with summaries and highlighted evidence, eliminating the need to browse hundreds of pages manually.
Health plans deploying these tools report up to a 50 percent reduction in average case review time. AI-assisted systems enhance consistency and reduce cognitive overload for UM staff, while preserving human oversight for critical decisions.
Regulatory Alignment: Meeting CMS Requirements Efficiently
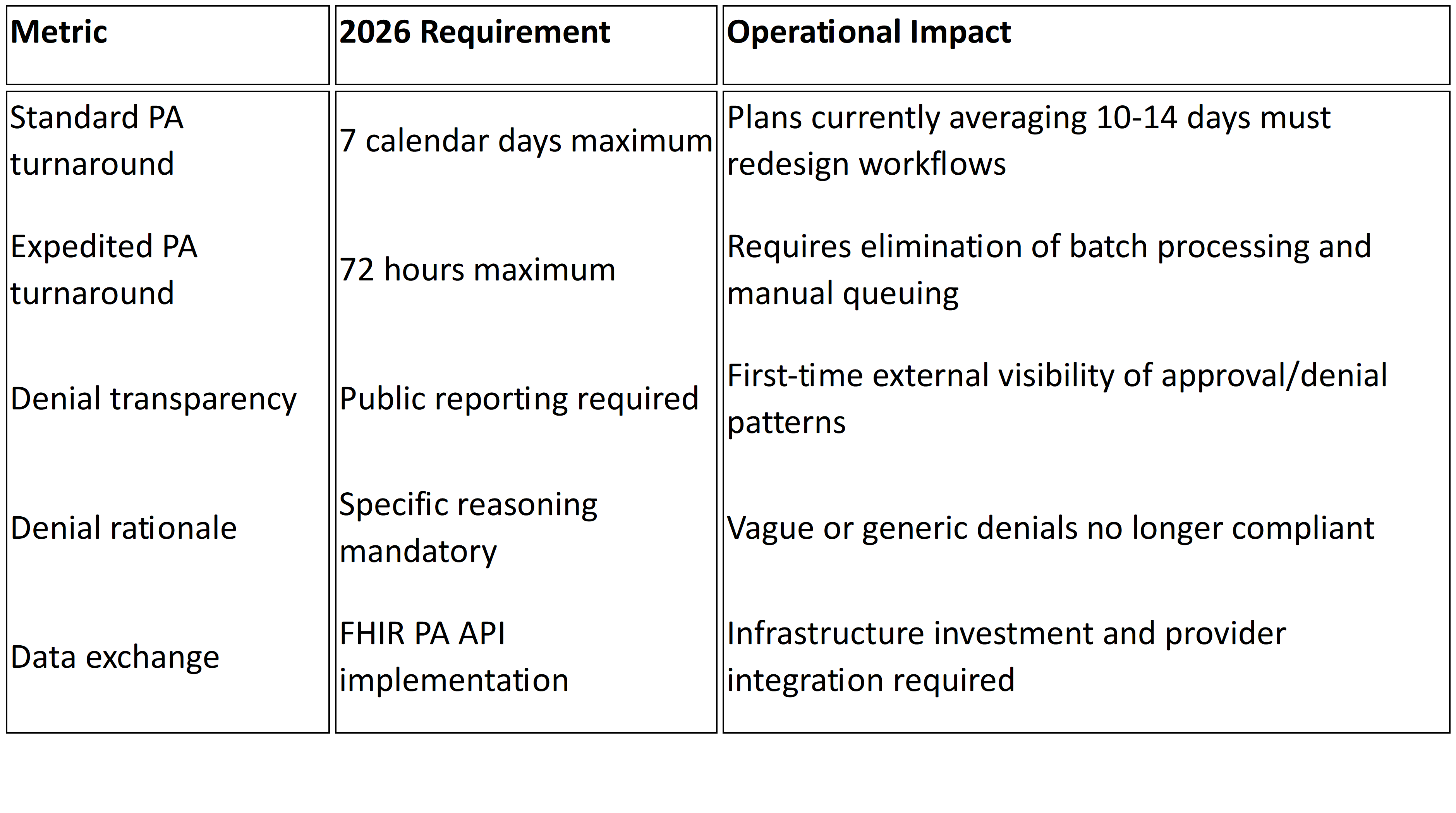
The CMS Interoperability and Prior Authorization Final Rule (CMS‑0057‑F), effective January 1, 2026 (with APIs required by 2027), imposes strict requirements: seven‑calendar‑day turnaround for standard requests, 72‑hour turnaround for expedited requests, public reporting of authorization metrics, and standardized API-based communication4.
Automation is essential for compliance. Without it, health plans risk missing deadlines, misreporting metrics, and exposing themselves to regulatory sanctions. Automated intake and AI-supported review systems facilitate meeting timeliness standards, improve denial rationale transparency, and generate structured data required for public disclosures.
Operational and Strategic Returns
Adopting automation and AI in UM workflows delivers measurable operational and strategic advantages:
- Faster turnaround times, supporting regulatory compliance and enhanced provider/member experience
- Lower administrative costs, with per-case cost reductions from dollars to cents
- Improved decision consistency, reducing variability and appeal risk
- Better provider relationships, fostering collaboration and satisfaction
- Scalable operations, capable of handling volume without linear staffing growth
According to CAQH projections, universal adoption of electronic PA could save the healthcare system nearly $500 million annually.
Governance and Change Management
Implementing automation successfully requires more than technology. Integration with core UM systems such as QNXT or Facets is a prerequisite. Oversight mechanisms must be in place to audit automated decisions and ensure human review for denied cases. Clinician training is essential to shift from manual workflows to supervisory roles. Transparency—through AI outputs aligned to policy rationale—is critical for provider acceptance.
Monitoring key performance indicators—including intake accuracy, review time, first-pass approval rates, and provider satisfaction—is essential for evaluating ROI and guiding continuous improvement.
Conclusion
In today's healthcare environment, utilization management processes demand urgent modernization. Fragmented intake channels and documentation overload threaten decision efficiency, care quality, and compliance. Automation and AI offer pragmatic, scalable solutions that improve accuracy, reduce administrative friction, and enhance both provider and member experience—all while supporting regulatory alignment.
For health plan executives, investment in intelligent UM is not optional; it is a strategic imperative. At Mizzeto, we partner with plans to deploy integrated technology solutions that optimize intake, augment clinical review, and embed rigorous governance. To explore a tailored blueprint for digitally transforming your UM operations, contact us today.
Sources Cited
2Administrative Transaction Costs by Provider Specialty
3Navigating The CMS Prior Authorization Final Rule: What Health Plans Need to Know
4CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F)